Osteoarthritis (OA) is the most common degenerative joint condition, affecting millions globally. Current treatments like medications, injections, and surgery often provide only short-term symptom relief. Photobiomodulation therapy (PBMT), also known as low-level laser or light therapy, is emerging as a safe, non-invasive option for reducing pain and inflammation while supporting cartilage health. This article reviews recent evidence on PBMT, including details on wavelengths, follow-up periods, and its role alongside regenerative treatments like stem cell therapy.
Methods: Wavelengths and Follow-up
The reviewed studies used PBMT at wavelengths ranging from 632 nm (red light) to 910 nm (near-infrared light). These wavelengths are optimal for absorption by mitochondria in joint tissues. Treatment sessions varied from seconds to minutes, with protocols repeated multiple times per week in animal and in vitro models. The average follow-up period across the included studies was up to 8 weeks. Pain relief, inflammatory markers (IL-1β, TNF-α), and cartilage repair were the main outcomes measured.
Results: Pain Relief, Inflammation, and Cartilage Repair
PBMT consistently improved outcomes in both animal and cell studies. Pain scores decreased significantly over time, showing a steady reduction from baseline to 8 weeks. Inflammatory cytokines such as IL-1β and TNF-α were reduced, while cartilage-building proteins like collagen type II increased. When PBMT was combined with mesenchymal stem cells, the benefits were amplified, suggesting a synergistic effect between light therapy and regenerative medicine.
The following graphs highlight key findings from PBMT research:
PMBT Pain Reduction Over Time
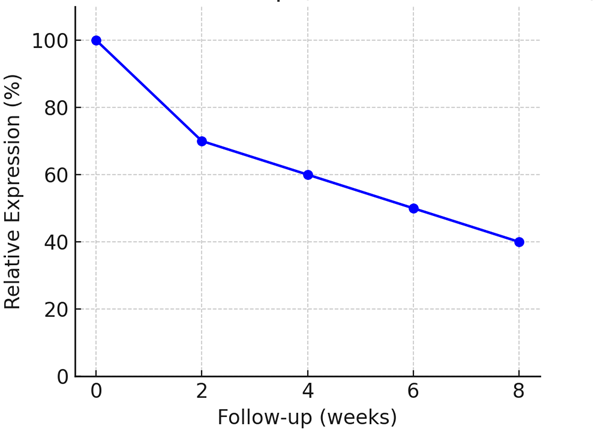
PMBT Effect on Inflammation Marker
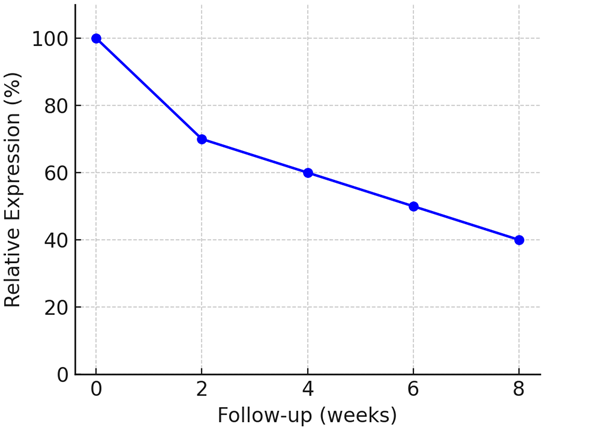
PMBT Effect on Collagen Type II Expression
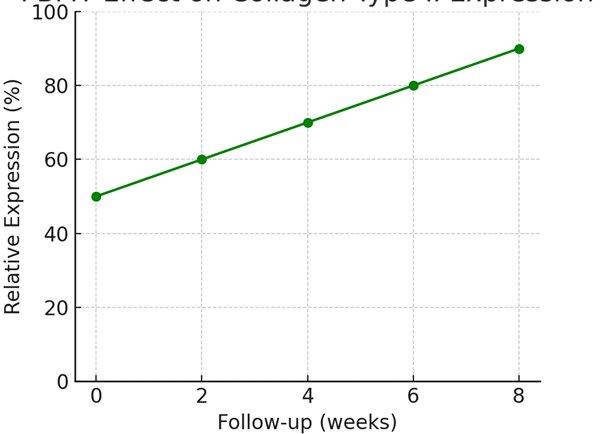
Why PBMT Matters in Osteoarthritis Care
OA is traditionally managed with painkillers, injections, and joint replacement surgery, all of which have limitations. PBMT offers a non-invasive, drug-free option that targets the cellular drivers of OA. By improving mitochondrial function, PBMT boosts tissue repair, reduces oxidative stress, and promotes cartilage regeneration. This represents a paradigm shift in how we think about managing chronic joint disease. Although this research is early and not done in humans with arthritis, it is promising and may help to provide an additional conservative treatment option that can be used in conjunction with biologic therapy like PRP and stem cells.
The Regenexx Difference
At Regenexx Cayman, advanced regenerative treatments, such as culture-expanded mesenchymal stem cells (MSCs) are combined with complementary therapies. PBMT may serve as a supportive modality, enhancing the effects of stem cell or PRP injections by improving cellular energy and reducing inflammation. This integrated approach underscores Regenexx’s commitment to offering world-class, evidence-based regenerative medicine.
💡 Thought Question: If a simple, non-invasive light therapy could slow down or even reverse joint degeneration, should it be offered alongside standard treatments for osteoarthritis?
Take the Next Step
If you or a loved one is living with pain caused by osteoarthritis, Regenexx Cayman offers advanced regenerative procedures that are supported by science. Our evidence-based approach integrates stem cell therapy, PRP, and complementary modalities like PBMT to reduce pain and restore mobility and quality of life.
Contact Regenexx Cayman today to explore your options. Call us on 345-943-5900 (Cayman) / 1-877-211-3834 (US Toll-free), or email info@regenexxcayman.ky.
References